
* The title of this presentation is aortic stenosis and low flow state, implications for diagnosis and treatment

* Degenerative aortic stenosis is the third common heart disease after hypertension and coronary heart disease in developed countries in the aging population

*Inconsistency between transvalvular mean pressure gradient and the Aortic valve area is one of the important challenges in severe aortic stenosis.

*In high gradient severe AS there are clear cut values like aortic transvalvular velocity more than 4 m/s and/or mean transvalvular pressure gradient ≥40 mmHg; the aortic valve area is typically ≤1 cm2 but only 50 % of the patients with symptomatic severe aortic stenosis patients are in this category
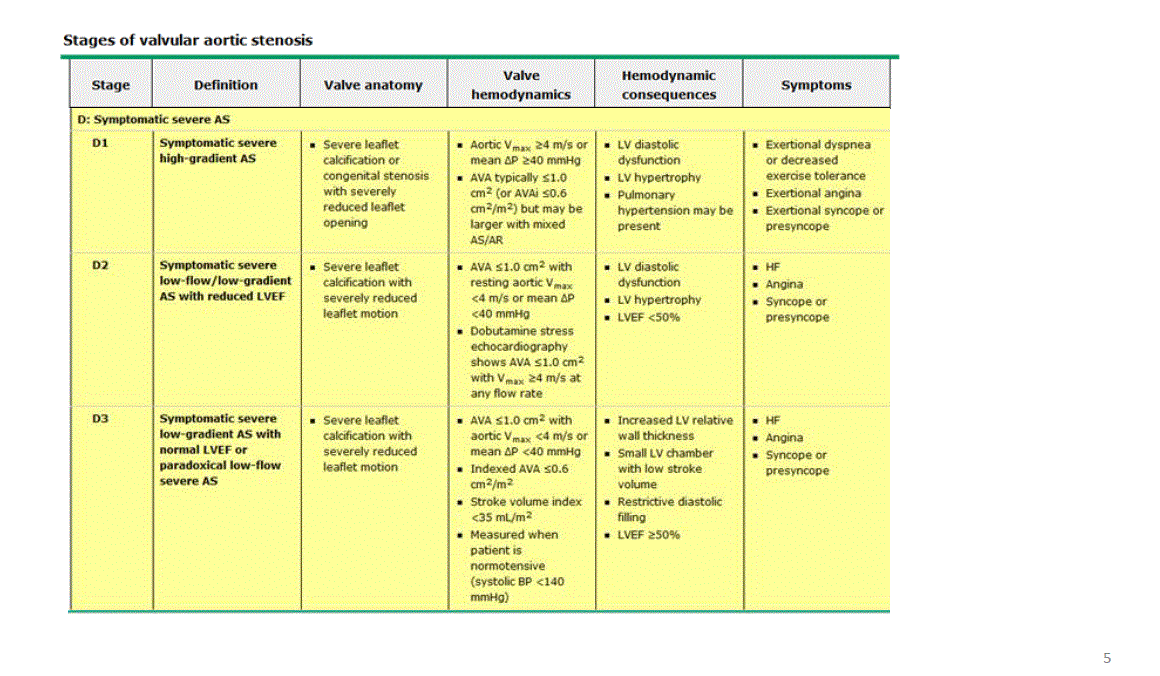
*Nearly half of the symptomatic severe AS patients are low gradient patients and most of them are low flow patients staged as D2 and D3 group in the guidelines
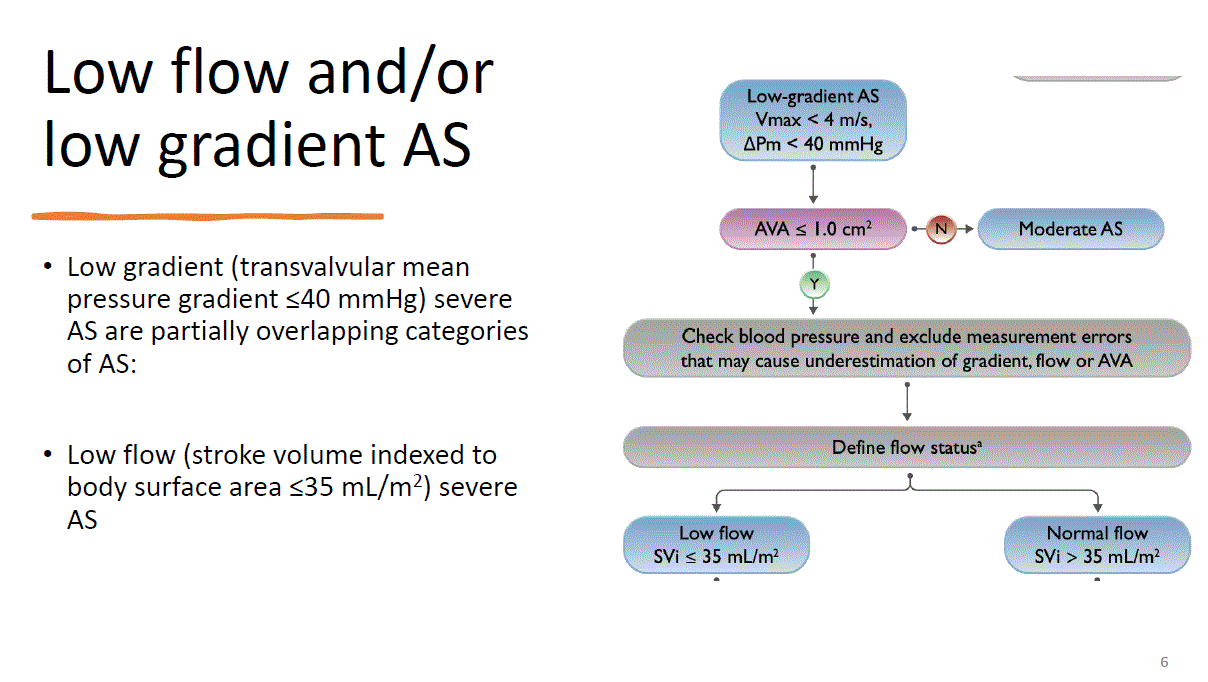
*When we talk about low flow we are also talking about low gradient, because according to guidelines stroke volume index measurements are required in patients with AVA less ten 1 cm and mean gradient less the 40 mmHg. If stroke work index is less then 35 the patient has low flow, low gradient aortic stenosis.
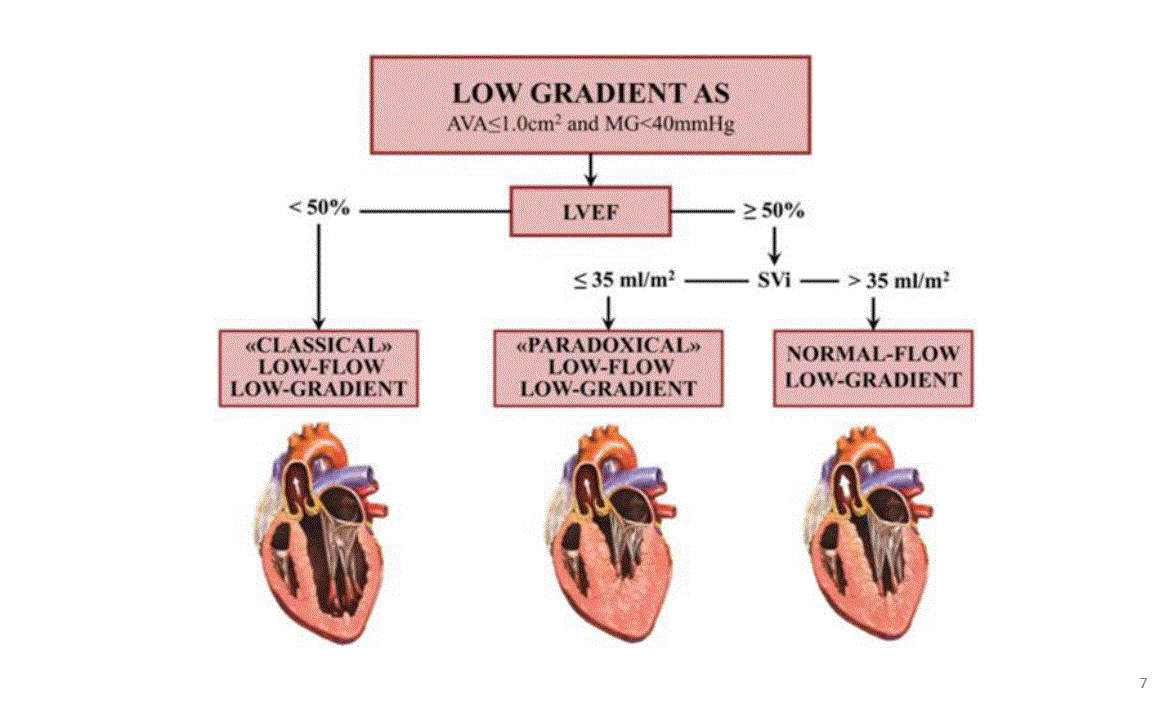
*If low flow patient has EF less then 50 % we are talking about classical low flow low gradient patients in which there is a dilated ventricle and some degree of mitral regurgitation. And if the EF is more than 50% in low flow patients, they are the paradoxical low-flow low gradient patient mostly hypertrophied restrictive ventricle is the reason for low flow. Normal flow low gradient patient patients are another topic for now we can accept them as moderate AS patients

*In these patients, we must decide if they have true AS in which the primary problem is the stenotic valve. They have low gradient because of low flow. These patients will benefit from aortic valve replacement.

*In pseudosevere AS, Valve problem is mild to moderate. The reason for low valve area is the low flow which can not fully open the aortic valve

*In classical low flow low gradient aortic stenosis in which EF is less ten 50% we know that we must perform dobutamine stress ECHO
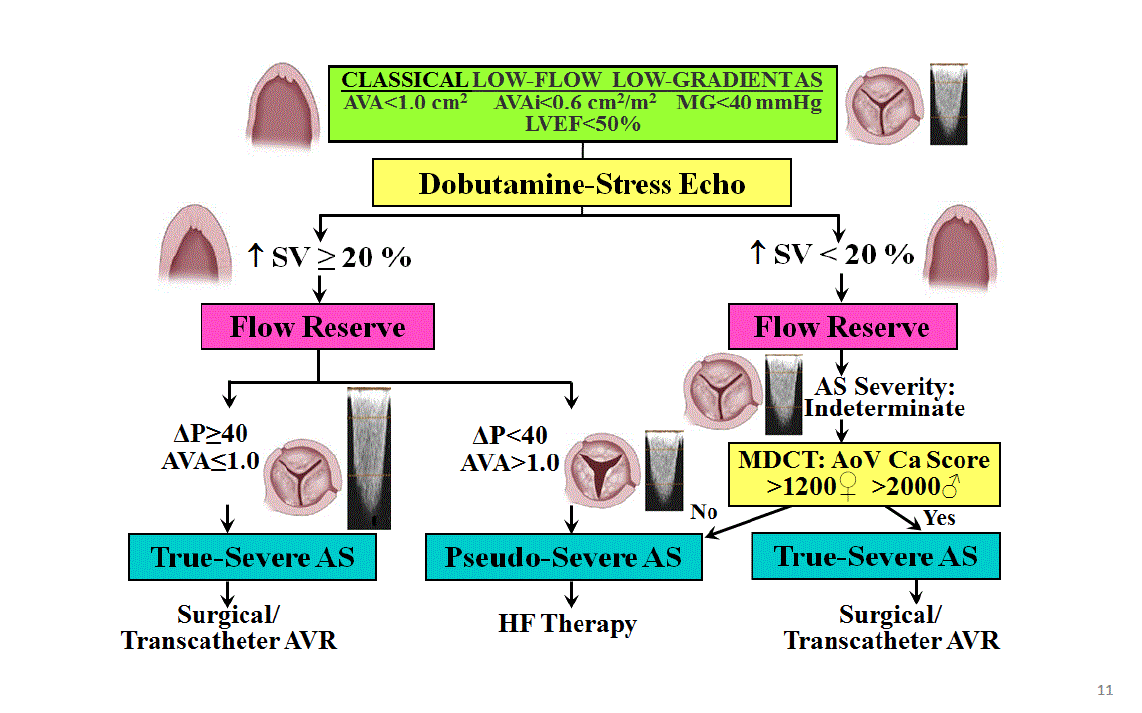
*In stress ECHO if stroke volume (flow reserve) rises more then 20 % it is easy to differentiate true from pseudo stenosis. In the true AS mean gradient rises without an enlargement in valve area. In pseudo AS mean pressure falls and valve area enlarges. The biggest challenge is the patients with some flow reserve but less then 20 without a change in pressure or valve area.
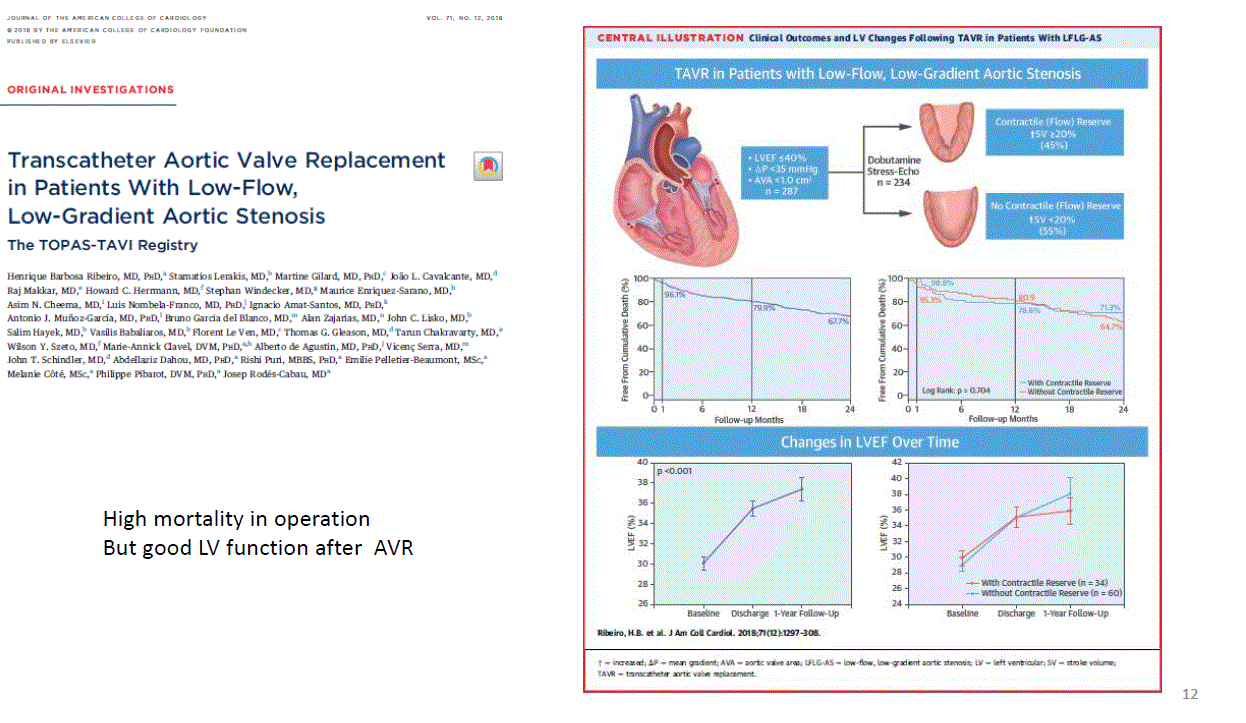
*If we decide to change the valve in these patients, we know that they will have a high operative mortality, but they will benefit nearly the same as the patients with flow reserve.

*It is recommended to perform CT for calcium scoring in these patients, to decide if they have severe stenosis and if Agatson unit is high aortic valve replacement is recommended.

*There are other ECHO techniques like projected valve area, and some clinician value this measurement as a combination with calcium CT scoring.
 *But it is not in the guidelines TOPAS III trial is invastigatin the value of this technique.
*But it is not in the guidelines TOPAS III trial is invastigatin the value of this technique.

*But dimensionless velocity ratio is in the American guidelines, and values less then 0.25 is valuable to differentiate true AS
 *In paradoxical low flow patient with EF more then 50% we have a step approach to determine if the patients have true AS. First the patients should be symptomatic AS patients
*In paradoxical low flow patient with EF more then 50% we have a step approach to determine if the patients have true AS. First the patients should be symptomatic AS patients
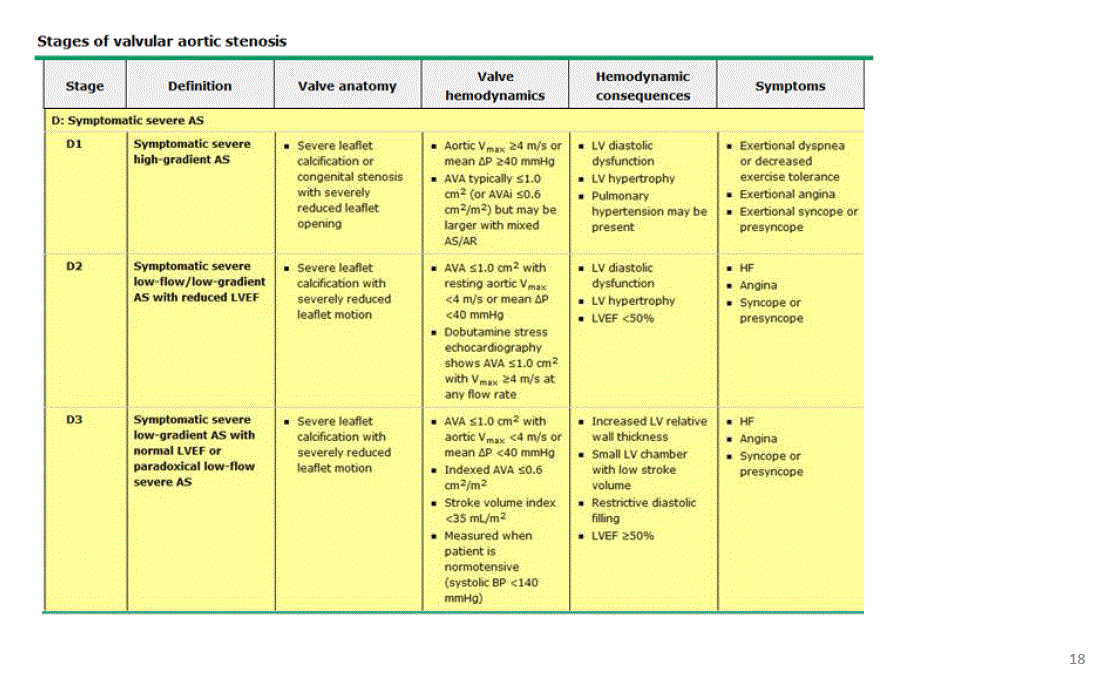
*Only the patient with symptoms and low flow low gradient is staged as severe AS

*If the patients are symptomatic then we must check if the ECHO measurement were made when the blood pressure were below 130 mmHg at the time of ECHO measurement.


*Both the European and the American guidelines do recommend optimization of the blood pressure before ECHO in low flow low gradient patients.

*If the Blood pressure is OK and we still have low flow low gradient we should assess other factors that can affect the flow like AF. Because we do measure mean of 5 waves in AF some are high, and some are low. AF can be the reason for low flow.

*In low flow low gradient patients with normal EF we must be suspicious about amyloidosis. Approximately 10-20 % of the patients will have wild type transthyrein amyloidosis. These patients will have bad prognosis if they have aortic valve replacement. And this disease has a specific treatment.

*Again, CT calcium scoring is the best tool in paradoxical low flow low gradient AS for the differential diagnosis of true AS
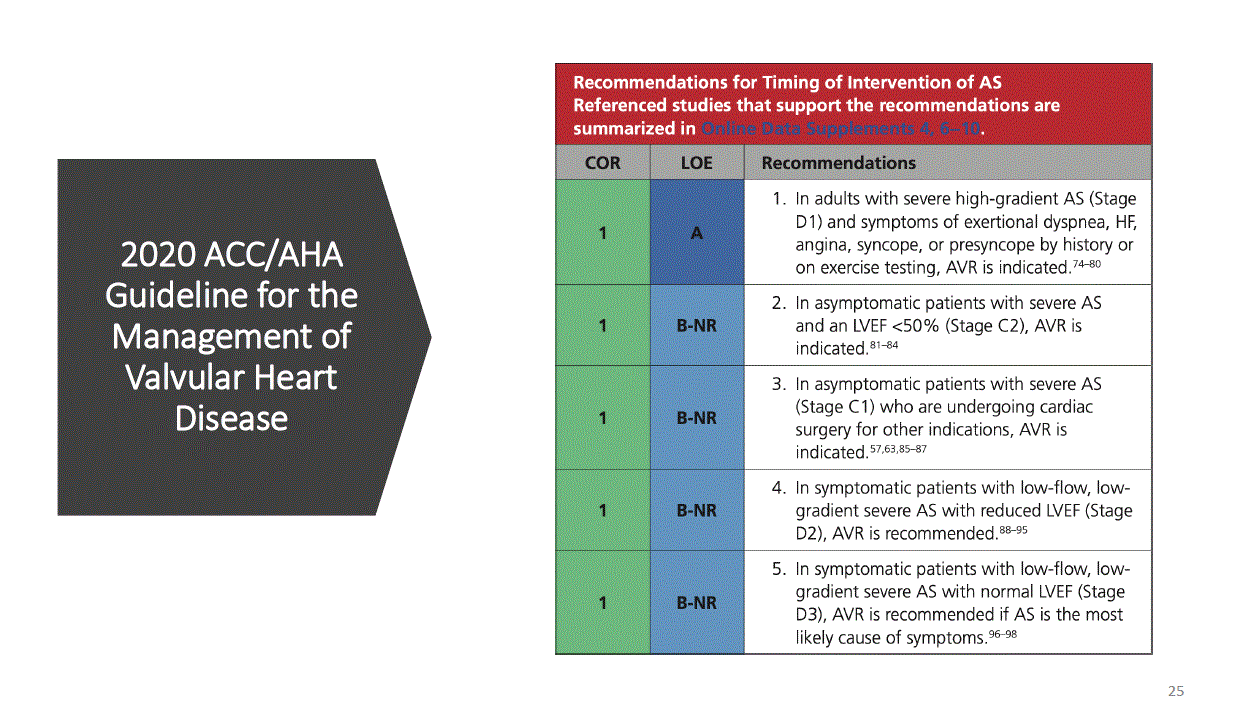
*In American Guidelines aortic valve replacement is class I indication for symptomatic classical low flow low gradient and paradoxical low flow low gradient AS patients if they have true AS

*ESC guidelines are more suspicious about paradoxical low flow low gradient AS, and classical low flow low gradient with no flow reserve. They are Class IIa recommendations.
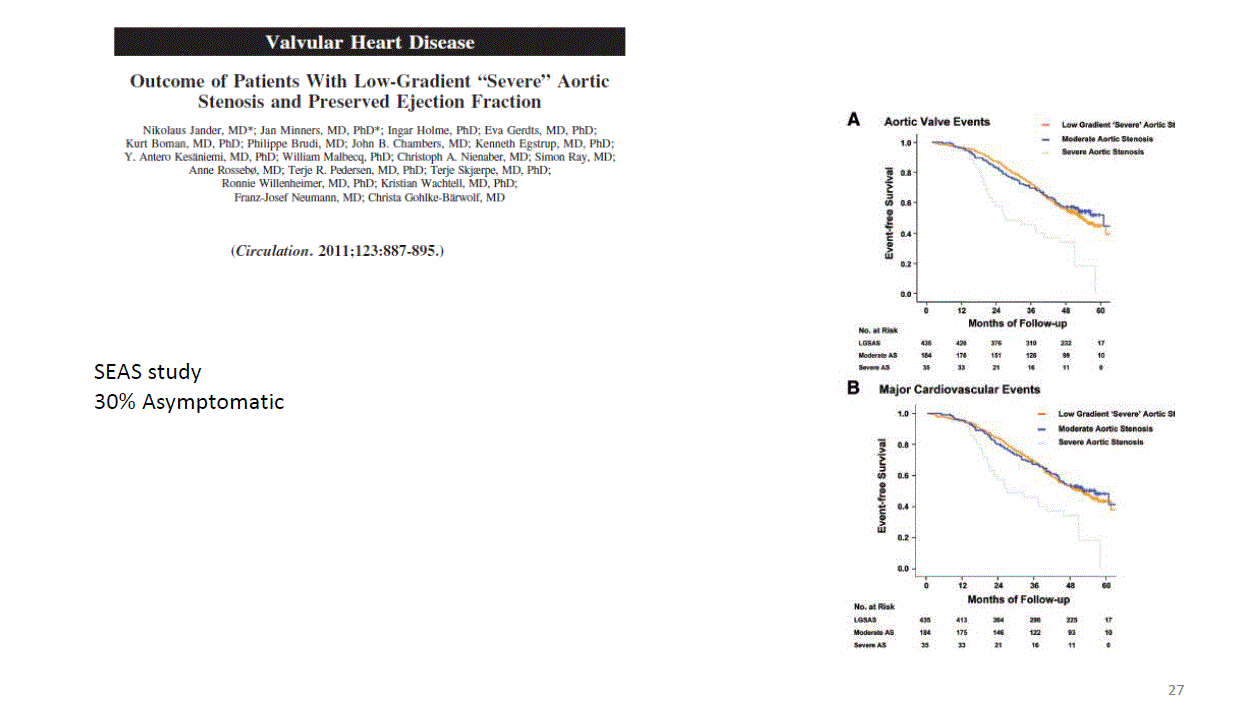
*One of the reasons for this is the early studies like, SEAS study in which the prognosis of paradoxical low flow low gradient patients was similar to moderate AS patients. But in this study 30 % of the patients were asymptomatic.
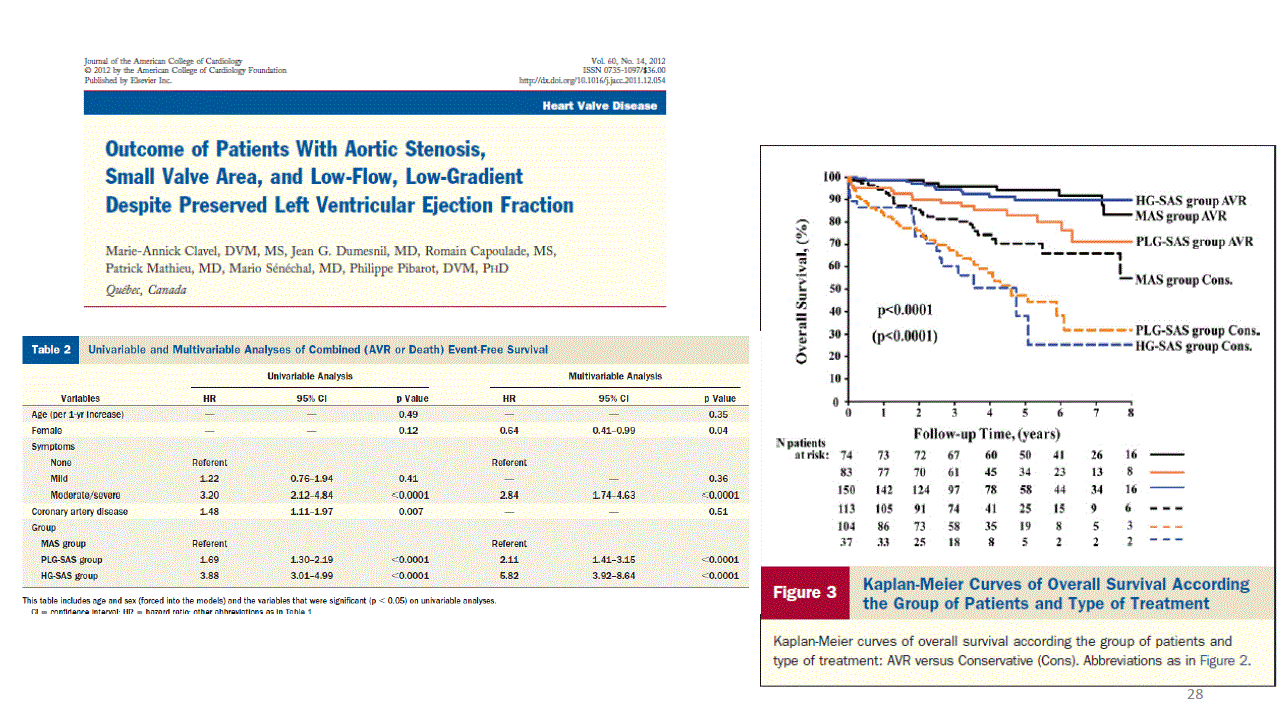
*But in the following years it is shown that after AVR these patients do not have good results like high gradient patients but if we go on conservative treatment their prognosis is bad as high-grade AS.
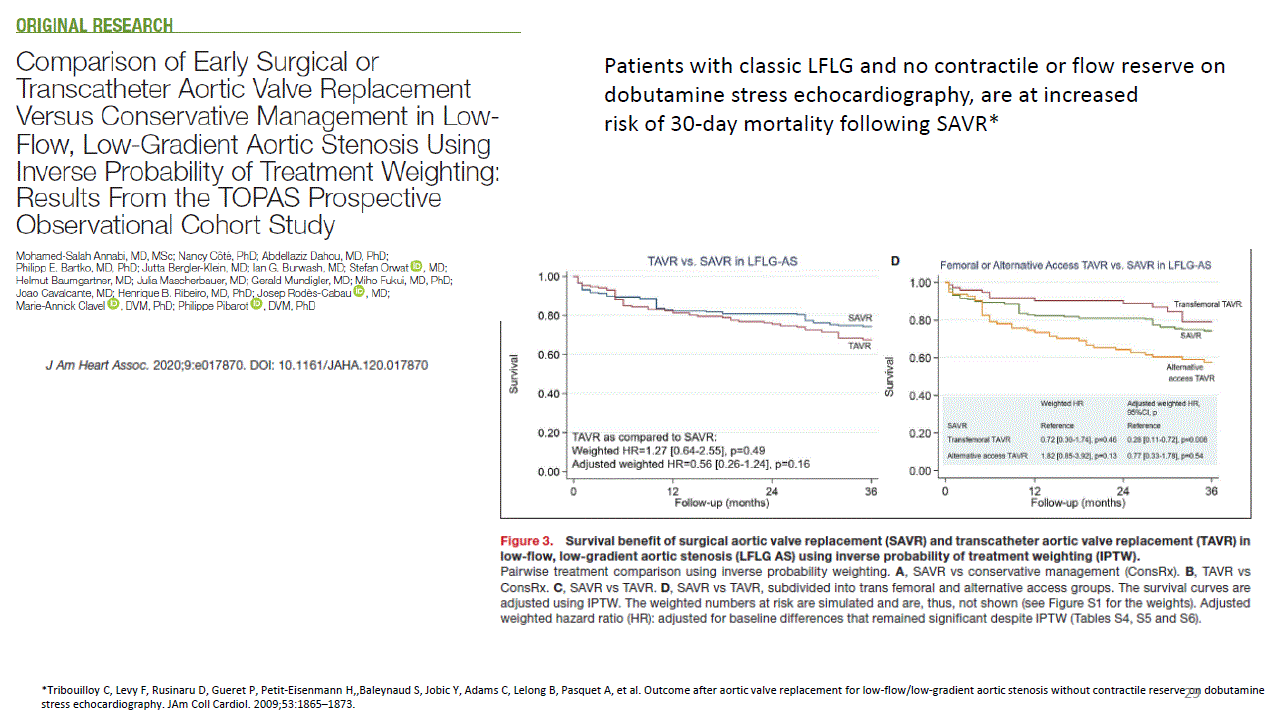
*And what is the best treatment for low flow low gradient patient surgery or TAVR. Patients with classic LFLG and no contractile or flow reserve on dobutamine stress echocardiography, are at increased risk of 30-day mortality following surgery. In overall in the univariate analysis there is no difference between surgery and TAVR but we should not forget that high risk patients are treated with TAVR if we normalize these values TAVR can be a better choice in these patients.